Highlights
| New Features | Enhancements |
|---|---|
| Even More Universal Import Updates | New Referring Provider Column in Claim Control |
New features
Even More Universal Import Updates!
This release introduces further enhancements to the Universal Import feature, continuing to streamline the mapping of imported columns to CollaborateMD fields. Key updates include:
- Recognizing institutional claims: Previously, customers were required to include a claim type column in their imports to specify institutional claims. This necessitated manual intervention, as EHR exports typically lack this information. This release introduces support for importing institutional claims by automatically identifying them through specific data fields. Fields such as Revenue Code, Value Code, Admit Type, and Condition Code are now used to recognize institutional claims, eliminating the need for adding a manual claim type column.
- Better Provider Name matching: We have improved our provider name matching. Provider names often appear in a single column, sometimes accompanied by IDs or credentials. In this release, the system has been updated to ignore these extraneous details to accurately identify the first and last names for searching. While the system now effectively parses these columns, we still recommend maintaining a separate provider NPI column whenever possible.
- Support for Different Modifiers for each charge: The system has been updated to support distinct modifiers for individual charges. Previously, the system incorrectly consolidated all modifiers into a single list and applied it to every charge. This release ensures that imported files correctly match specific modifiers to their respective charges. Additionally, the system now treats "NA" or "N/A" values as blanks when multiple modifier codes are present.
- Support for State's Full Name: We have updated our address matching to support both full state names and two-digit abbreviations. The system now correctly processes EMR files regardless of whether the state is provided as a full name (e.g., Florida) or an abbreviation (e.g., FL).
- Better Recognition of columns with duplicate or invalid values: We have updated the system to improve handling of multiple potential matches, such as when both rendering and provider NPIs are submitted. The system now clearly distinguishes between matched and unmatched entries. Previously, if one field matched, the other was omitted, which often caused confusion regarding the data imported.
- Improvement when combining multiple rows into one claim: Previously, the system consolidated rows for the same patient based solely on claim or appointment IDs. This often incorrectly merged records involving different providers or payers. Because distinct providers indicate separate services, these records must remain on individual claims. This update improves logic to prevent the improper combination of claims.
- Excel formatting now used for number columns: When exporting member IDs starting with zeros to Excel, the application often removes the leading zeros, resulting in incorrect IDs and claim denials. In this release, we updated the Excel formatting for numeric columns to preserve leading zeros.
- Support for Importing Patient's Marital Code: Resolved an issue where patient marital status failed to import during data retrieval for meaningful use or other tracking purposes. This release ensures the information is now correctly imported.

Continue checking our release notes for further Universal Import updates and enhancements coming soon.
Enhancements
New Referring Provider Column in Claim Control
When reviewing claims, users often need to verify referring provider information, particularly for services or payers where the referring provider is always required. Previously, when working claims from the Claim Control screen, users had to open each individual claim to ensure this information was present and accurate. To improve this workflow, we have added the referring provider as an optional column (hidden by default) in Claim Control. This column allows users to identify and quickly access claims missing a referring provider for correction.
GPI Onboarding Now Automatically Checks Status of In-Progress Applications
Previously, the status of in-progress GPI applications (and their credentials) was only checked when users manually accessed the In-App Payment Processing section. As this process was often overlooked, we have updated the system to automatically check for pending applications upon login. This ensures that credentials and merchant details are retrieved promptly, allowing users to begin processing payments without delay.
Resolutions
Ability to Run Patient Eligibility When a Patient Record is Locked
Previously, if a user opened a patient record already locked by another user, they could view the information but were unable to check eligibility. As saving the record is not required to perform this action, this update allows users to run eligibility checks even when a patient record is locked (in use) by another user.
Practice Fusion Issues Fixed
We also implemented reliability improvements to resolve a duplication issue where Practice Fusion sent redundant claim copies.
Scrolling Issues in Safari
We have resolved scrolling issues in Safari where headers would disappear when viewing large tables. The headers now remain correctly positioned. Mac users who previously switched browsers due to this issue may now return to Safari, as functionality has been restored.
Intelligent Claim Rejection: "Marked as Fixed" Issue
We resolved an issue where marking claim rejections as "fixed" did not consistently update their status. Previously, claims remained visible in search results for unresolved issues due to underlying errors that were not properly cleared. This update ensures that all claim issues are fully marked as resolved upon confirmation.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| New Features | Enhancements |
|---|---|
| More Universal Import Updates | New GPI Onboarding Tooltips Revenue Code-Specific Taxonomy Codes |
New features
More Universal Import Updates
This release introduces further enhancements and updates to the Universal Import feature, streamlining the process of mapping imported columns to CollaborateMD fields. The system now supports importing addresses consolidated into a single column by automatically recognizing individual address components (street, city, zip, etc.). Additionally, we have added support for importing multiple insurance policies from a single column to accommodate various export formats. Please note that we still recommend keeping address fields such as street, city, state, and zip code in individual columns whenever possible.
This release includes updates to ignore "N/A" fields in columns, eliminating the need for manual removal prior to upload. We have also improved payer name matching, allowing files to be uploaded without editing names containing extra parentheses or special characters. Additionally, refinements to the AI prompt will minimize unexpected errors during file imports. 
Continue checking our release notes for further Universal Import updates and enhancements coming soon.
Enhancements
New GPI Onboarding Tooltips
Several sections of the GPI In-App Payments application have caused customer issues; for example, entering incorrect placeholders for average transaction amounts has led to application delays or denials. In this release, new tooltips have been added to the merchant details screen during GPI onboarding to clarify these fields. Hovering over these fields now displays a tooltip explaining the required information. Tooltips have been added to fields such as types of goods, services, annual volume, average sale price, and sales channels, to assist customers in completing the required information.
Revenue Code-Specific Taxonomy Codes
Vermont Medicaid requires specific taxonomy codes for certain behavioral health institutional claims, depending on the revenue code used. To comply with these billing guidelines, a new "Taxonomy Code Override" field has been added to the Revenue Code section within the Claim Defaults tab. This allows users to assign specific taxonomy codes to individual revenue codes.
Please note that this feature requires a feature flag. If you require access to per-revenue code taxonomy overrides, please request it via a support case.
Resolutions
Claim Control Incorrect Warning
Some users previously encountered warnings in Claim Control when a claim contained charges with multiple statuses. Because the system's ability to update these statuses depended on the things like the processing order, the behavior was inconsistent and confusing.
In this release, we resolved this issue so that Claim Control now correctly processes charges regardless of their individual statuses within a claim.
Incorrect Warning for "Forgot Password" option
New Institutional Claim Edit: TOB 86x
We have added a new institutional claim edit for bill type 86. These inpatient claims generally do not involve a hospital admission; therefore, by default, we do not transmit admitting diagnoses or related admission fields. If customers using bill type 86X experience rejections or denials due to missing admission information, they may request this edit via support. We can then enable their payer to ensure the admitting diagnosis is included when the bill type begins with 86.
Custom Edits (Aptarro) Issue
We resolved an issue regarding custom edits at Aptarro where certain submitter IDs were missing from our system despite being previously established. All affected submitters have been corrected, and we have implemented measures to prevent submitters from being inadvertently removed in the future.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| New Features | Enhancements |
|---|---|
| New Total and Selected Patient Counts in Claim Control | Payment Automations UI Update Universal Import UI Update |
New features
New Total and Selected Patient Counts in Claim Control
We previously added the total and selected charges & claims to the bottom of the Claim Control results screen. In this release, we added "Total Patients" and "Selected Patients" counts to the Claim Control results screen. These fields display the total number of unique patients and, when claims are selected, the number of unique patients within that selection.

Enhancements
Payment Automations UI Update
The "Edit" button previously located at the top of the payment automation screen was misleading. Rather than allowing users to modify specific automations, this button is used to reorder, activate, or deactivate them. To edit an individual automation, users must open the specific entry directly. To avoid confusion, in this release the "Edit" button within Payment Automations has been renamed "Reorder," as it is used to reorder, activate, or deactivate automations rather than edit them. 
Improved Deposit Date Reporting
We have improved the performance of reports, such as the Daily Deposit Report, when filtering by deposit date. Previously, generating these reports for large accounts over extended periods was time-consuming. By adding an index to the Deposit Date field, we have matched the efficiency of reports filtered by received date, significantly increasing processing speed and preventing timeouts.
ERA Negative Adjustments
Previously, negative adjustments were not applied correctly to ERAs, resulting in inaccurate credits. This issue pertains to scenarios where a payer’s payment and adjustment total exceeds the billed amount, adding a negative adjustment (not refunds/reversals). In this release, the system has been updated to correctly apply these negative adjustments for primary payers when claims are received with amounts intended to offset overpayments.
Universal Import UI Update
We made a minor update to the universal import process. Previously, after reviewing the field matching in the review screen and then selecting " import" the dialog remained open, requiring users to manually close it to see the option to review the results. With this update, the dialog now closes automatically, removing an extra step and streamlining the workflow. 
Resolutions
Electronic Statements Issue
We resolved an issue where setting up electronic statements when the patient was already receiving paper statements, would occasionally received both formats simultaneously, exceeding the established statement limit before an FDN. In this release, we updated the system so that enabling electronic statements for patients already receiving paper statements will not trigger electronic delivery for them. Electronic statements will now only be issued to patients who have not previously received paper statements. Once a patient pays and resets their balance, the process restarts: we will send electronic statements, followed by paper statements and the FDN.
Incomplete Claims Won't Appear in Follow-Up Management
Interface Error With the Archive Insurance Option
We previously identified isolated interface errors that prevented claims from posting and patient records from updating. As a workaround, users were advised to temporarily disable the "archive patient insurance information" setting. This release resolves the issue, allowing users to re-enable this feature.
Universal Import Updates
Invoice Email Update
Resolved an issue where users incorrectly received invoice emails after being reassigned from a custom permission to a "User Role" without the permission. The system had failed to clear the legacy permission, causing it to persist despite the role change not including it.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| New Features | Enhancements |
|---|---|
| Universal Import | New Rich Text Editor New Automation for Value Code 80 |
New features
Universal Import
This release introduces the beta version of CollaborateMD's Universal Import feature. Many Electronic Health Record (EHR) systems now include interfaces designed to export data, often in HL7 standard format, offering greater flexibility to their users. However, a common issue is that numerous EHRs lack interfaces for external systems. This deficiency creates substantial additional work for medical practices and billing services, as they are forced to manually input claims and patient data into CMD.
Our Universal Interface Import allows users with an EMR/EHR that has not built an interface with us to import encounter, claim, and patient data from any external system. Customers can now upload CSV, Excel, TSV, and pipe-delimited files using our Interface Import section. This new feature uses AI-powered field mapping to automatically interpret the structure of CSV/Excel files from other systems and map them into CMD. This feature allows customers who do not use our WebAPI to automatically import claims, and patients from any EMR/EHR via a report or export from their software. 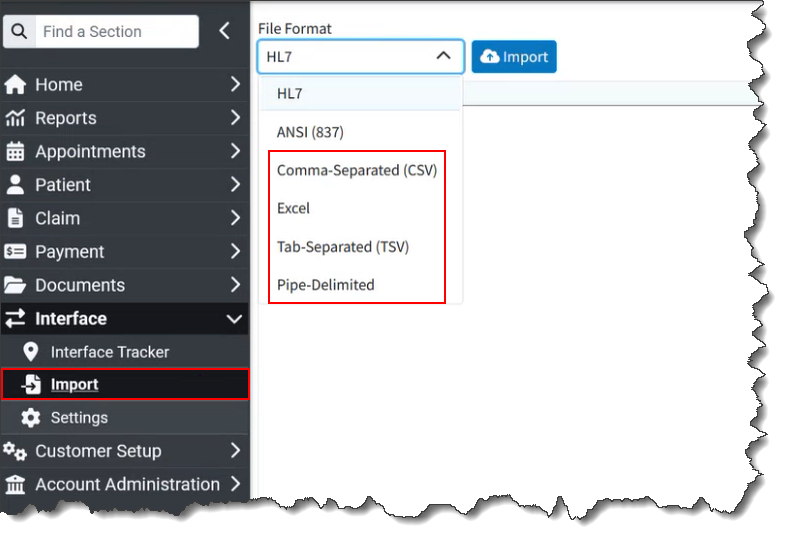
Customers can still manually import claims into our system in the HL7 format or from an 837 ANSI file into CollaborateMD.
For more information visit our Universal Import Help Articles or visit our Universal Import Interactive Demo.
Enhancements
New Rich Text Editor
This release includes an update to our Rich Text Editor, used in sections such as alerts and messaging. Although the editor functions similarly, you will notice some changes to the toolbar's appearance and its items. Icons for bold, italics, underline, and insert link remain largely the same, while others, such as Font and Font Size, have a new look. The previous Text Color and Highlight Color icons were combined into one. The Indent, Insert Ordered List, Insert Unordered List, and Insert Table icons are now visible in the toolbar. This new editor reduces clutter and increases visibility directly from the toolbar.
New Automation for Value Code 80
We previously added the ability to default value codes at the payer and patient level for institutional claims as part of our claim workflow enhancements. Value codes are specific billing details on institutional claims. For example, value code 80, "Covered Days," represents the number of days covered by the bill. This value will vary per claim, so it should not be set as a default amount.
In this release, we added an automation for value code 80. When value code 80 is used, leaving the amount blank in the default value codes section for the payer or patient will change the value field to "number of days" instead of "dollar amount." Subsequently, when a claim is received via interface, the value code's amount will be automatically set based on the number of covered days. 
Resolutions
ERA Reversal Matching Improvement
We resolved an issue that prevented some ERA reversals from applying correctly. The affected ERAs received a "we couldn't apply the reversal because there was no prior reversal to apply to" warning message. With this update, the system now looks at the previous payment to determine how the payment and adjustment should be posted. This ensures consistent application, allowing reversals to be matched appropriately.
Corrected GPI Onboarding Issues
We fixed several issues with the GPI onboarding when setting up In-App Payment Processing. The "Percentage of Processing Methods" field will now have improved validation to prevent progression with invalid or null information. Additionally, the "Title" field for the Authorized Signer will now be a dropdown menu with allowed options, preventing errors, as GPI expects specific values.
Intake Forms: Unmatched Forms Option Fixed
We corrected an issue with our Intake Forms' "Unmatched" forms feature. A previous release accidentally created a bug that prevented the option to fix unmatched intake forms from appearing when clicking on an "Unmatched" form. This has been corrected in this release and is working again.
Incorrect Net Amount Issue
We resolved an issue where a net amount could be calculated incorrectly for patients. This issue prevented the charge-level allowed and net amounts from calculating correctly in the daily/monthly net charges report. Although this issue will be fixed going forward, existing patients may still have invalid values. If that is the case, opening and saving the patient will solve the issue.
Multiple Universal Import Beta Fixes
Since releasing the Beta version of our Universal Import feature, we have updated and corrected some issues. First, we updated the Universal Import user interface to simplify the process and improve readability. We also updated how Universal Import files are read to better determine header and value rows. This means users do not need to remove blank or additional rows before the file header.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| New Features | Enhancements |
|---|---|
| New Plan Name Details Within the Eligibility Plan Number | ERA Name Mismatch Warning Will Now Ignore the Middle Name |
New features
Eligibility Will Now Show Extra Details Within the Plan Number
This item has been delayed due to a bug but will be released soon.
Accurately identifying a patient's plan is important for any practice, but it is critical for California IPA plans. In California, Independent Physician Associations (IPAs) are often tied to specific medical groups and PCP networks. The plan number acts as a code to identify the exact health plan and managed care plan network, which directly dictates patient benefits, PCP assignment, and required authorization procedures for services. When we receive an eligibility response message, it sometimes includes an additional segment with the name of the Group, Plan, or Network associated with the plan number.
In this release, when the eligibility response message includes an additional segment with the group, plan, or network name, we will now include the plan name when it is provided with the plan number in the response. This will assist practices that handle California IPAs by offering an additional reference point to minimize errors. 
Enhancements
ERA: Name Mismatch Warning Will Now Ignore The Middle Name
When reviewing an ERA, if a patient had a mismatched middle initial, the system would always display the "Name Mismatch" warning. This scenario could occur if the ERA and CMD records have a discrepancy in the middle initial, such as one record including it while the other does not, or if the initials themselves differ.
The purpose of this warning is to identify instances where the payer may have a completely different patient. A missing middle initial is not critical and was generating numerous warnings for correct patients due to unmatched or missing initials.
In this release, we updated this process to no longer show this warning based on the middle initial. Instead, it will only check if the first and last name do not match, regardless of whether the middle initial is present. This will reduce the time spent reviewing unnecessary warnings.
Resolutions
Missing Tooltip in Dashboards
A bug affecting the A/R Dashboards has been fixed. The bug, introduced in the last release, prevented the hover-over feature from displaying the amount represented by a bar or graph point. This functionality has been restored. 
Copy Configuration Issues Within Claim Scrubbing
When an authorized representative adds additional services, particularly for billing service customers, they can copy existing service configurations of certain services from one customer to another. This feature is crucial for billing services that frequently onboard new customers, as it significantly reduces data entry and setup times.
The problem was that the copy configuration feature was not working correctly for the "Claim Scrubbing" feature. When Copy Configuration was used for claim scrubbing, the selected specialty was not set up correctly, and the Aptarro submitters were not set up for the enabled customers.
In this release, we corrected this issue so that when the "Copy Configuration" option is used, the system copies and displays the selected specialty and registers the required submitters with Aptarro.
Copy Configuration Issues Within Interface Automation Settings
We also corrected an issue where, the copy configuration option was not working for interface automation settings. This meant that when copying the configuration to other customers, applicable interface automation settings, within features such as address verification and eligibility, were not being copied over.
In this release, we resolved this so that if there are any interface automation options selected, they are also copied over as part of the process. 
Claim Tracker: Mark as Fixed Issue
We also corrected an issue stemming from our 16.3 release, where Claim Tracker inconsistently marked some rejections as fixed. When checking the claim-level checkbox next to a claim without expanding it in Claim Tracker, the row would remain checked, but the "Mark as Fixed" and "Task" options would remain grayed out or unavailable. This was causing issues by selecting (checking) "Mark as Fixed" at the claim level instead of the issue level.
Global Period Alert Issue
The Global Period alert ensures the correct modifiers are used for post-surgery procedures. These procedure codes typically have a follow-up period during which charges for normal post-operative care are bundled into the global surgery fee. Therefore, when a claim is saved with a Date of Service (DOS) that falls within the global period of a code on a previous claim, the Global Period alert will appear to warn the user.
In this release, we fixed an issue where the global period alert was not appearing as expected under specific circumstances where, based on the modifier, it should have triggered the alert. We corrected the issue, and the feature now activates when any relevant modifiers are used.
Report Performance Improvements
A change was implemented in our report processor to significantly improve the performance of certain reports, depending on the filters used. Due to the nature of this change, it is difficult to predict which specific reports will experience performance improvements, but we should see better overall performance. It is important to note that this enhancement does not target a specific slow report. Instead, it addresses a pattern of report slowness issues observed within the application environment.
"Find a Time" Option Issue Within the Scheduler
We corrected an issue where the "Find a time" feature in the appointment scheduler did not consider appointment blocks. Appointment blocks are intended to prevent appointments from being scheduled within the blocked time. However, the "Find a time" feature was providing a list of available appointment slots that included times that should have been blocked.
This issue has been resolved in this release, ensuring that the appointment time-slot list provided via the "Find a time" option does not show appointment slots within blocks that disallow appointments. 
Updated Sending All Charges to Secondary Payer After a Payment
Previously, several changes and updates were implemented to ensure all charges are sent to the secondary payer after a primary payer payment. Although this is correct when there are other unpaid charges on a claim, it caused the system to send claims to the secondary payer even when all charges had been paid. In these scenarios, the secondary payer would have no action to take because the charges had already been paid by the primary. The secondary payer would then issue a $0.00 payment, rendering the claim submission inefficient.
In this release, we updated the system to ensure claims are not sent to the secondary payer if all charges are paid. This update will only send charges to the secondary payer if at least one charge has a balance greater than zero dollars ($0.00).
Family Statements: Printing Issue
When printing family statements, selecting "Family Statement" from the master account will generate a statement (Enhanced or Plain Text) for the entire family. However, if printing from a dependent's account with the "Family" option selected, only that dependent's statement will be printed.
In this release, we updated the system so that a family statement can now be printed from the dependent's account. This eliminates the need for users to switch to the master account to print a family statement.
Fee Schedule: Round Prices Up to The Next Whole Dollar Option Not Working
In this release, we updated the option to round prices to the next whole dollar amount (available when updating prices), which was previously not working correctly. With this update, when selecting the "Round prices up to the next whole dollar amount" option, procedure prices will now be correctly rounded up. 
Copay Credits Applied to Incomplete Claims
When copays are configured to auto-apply to claims created via interfaces, they should never auto-apply to incomplete claims. We previously found some instances where this occurred, so in this release, we updated the process to prevent copay credits from being auto-applied to claims with an incomplete status.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| New Features | Enhancements |
|---|---|
| Universal Import - BETA
|
New Option to Stop Showing the All-Inclusive Code Warning
|
New features
Universal Import Updated UI - BETA
Please be aware that the new universal import options are currently in BETA testing and will be available to all customers soon!
In this release, we updated the Universal Import user interface to simplify the process and improve readability. We enhanced it by removing unnecessary fields and clutter, renaming file naming conventions, automating the matching of existing templates, and converting mapped preview data into a table. This facilitates scanning either the header or CMD field to ensure accurate field matching.

For more information visit our Universal Import Help Article.
Enhancements
Claim: New Option to Stop Showing the All-Inclusive Code Warning
All-inclusive codes are common in Rural Health Clinics and Federally-Qualified Health Centers. In our system, entering a claim with an all-inclusive code triggers a warning. This notification indicates that an all-inclusive code has been selected and explains the impact on other charges. These charges will either not be billed or will be billed with a nominal amount, such as $0.00 or $0.01, depending on system configuration.
Because this all-inclusive code prevents users from editing other charges on the claim, the pop-up informs them that these are non-editable amounts. The problem is that this is inconvenient for some customers that work thousands of claims, when it happens for every claim.
To address this, a "Don't show this again" checkbox has been added to the All-Inclusive Code warning message in this release. Checking this box allows users to suppress the All-Inclusive Code warning dialog for the same user when editing or creating a new claim with an inclusive code.
 We also added a tooltip under the procedure description so that the information is still available without disrupting or prompting the user to close the warning.
We also added a tooltip under the procedure description so that the information is still available without disrupting or prompting the user to close the warning. 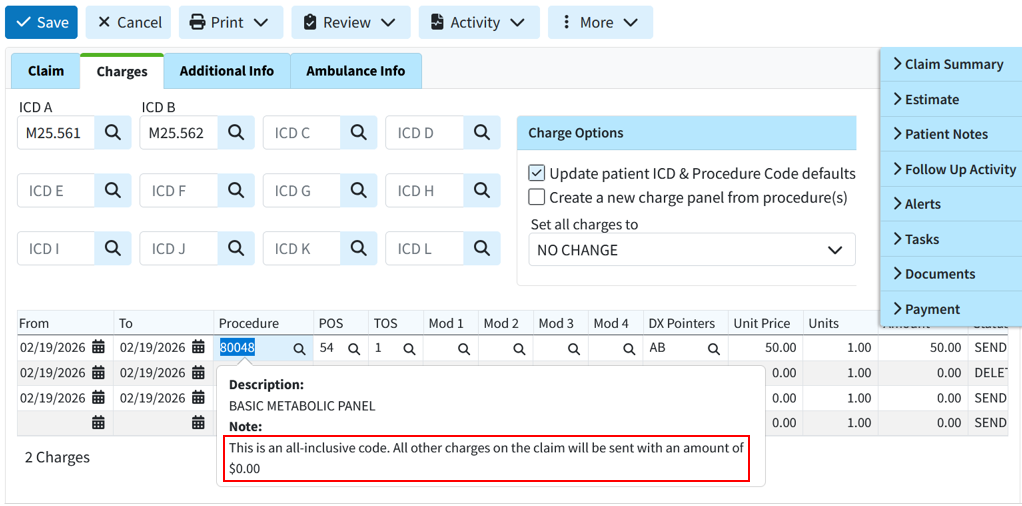
TCN Search Now Ignores the TCN Prefix
We recently added the submitter-level TCN Prefix feature to help the clearinghouse ensure that ERAs are routed correctly and to facilitate ERA splits.
This feature has been very helpful, but it could be inconvenient for some users depending on their workflow because if the full TCN, including the prefix, was copied from a payer report or EOB, users could not search for the correct claim or patient within the application. They would have to carefully copy the number while omitting the prefix, which could be difficult due to the small font on some reports.
In this release, the submitter-level TCN Prefix was updated so the system ignores it when searching by TCN in the claim, claim tracker, patient, insurance check, and ERA searches. This means that copying a TCN number from an EOB will no longer require partial selection for the search to function. This update allows the system to locate claims that include the prefix when copied.
Resolutions
WebAPI: Payer & Patient Default Value Codes Not Set on Claims
We have systematically implemented the ability to use more default codes from interface claims (such as value codes from revenue codes), but patient default codes and payer default value codes were still missing.
In this release, we are adding both Patient and Payer default value codes. When a claim is received via the API, the system will now add the default value codes in the following priority order:
1. Value Codes from the interface message (if sent)
2. Payer Defaults
3. Patient Defaults
4. Revenue Code Defaults
At each priority step, the system will only add value codes that have not already been included. For example, if the interface message sends value code 16, and the patient defaults include value code 16 and value code 18, then the message's amount for value code 16 will be used, followed by the patient's amount for value code 18.
Practice email address is automatically set as the "Reply-To" address for electronic statements
Previously, the practice email address was automatically set as the Reply-To address for electronic statements. Users were often unaware that the practice email was used as the default Reply-To email address when setting up their electronic statements, as this option is part of the electronic statement options. To prevent user error, we updated this release to default the Reply-To address to "No Reply," even when a practice email address is available. This will ensure that any Reply-To address set for electronic statements is added intentionally by the customer. Please note that existing configurations will not change. This applies only to electronic statement setups moving forward.
ERA: Incorrect Claim Status
Resolved an ERA issue that caused a charge balance with no additional payers to display an incorrect claim status. It showed a "PAID" status instead of "BALANCE DUE PATIENT," despite an existing balance and no other payers.
ERA & EOB: Incorrect allowed amount on refund/reversal
We corrected an issue within our ERA/EOBs causing an incorrect auto-calculation of the allowed amount on some refund/reversals.
Universal Import: Support First and Last Names with Spaces
We corrected an issue within our universal import detected during testing where names containing spaces but no hyphens, apostrophes, or symbols (e.g., "De La Cruz," "Van Dyke," "Mary Jane") were not recognized correctly during import.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| New Features | Enhancements |
|---|---|
| Universal Import - BETA
|
New Option to Ignore Modifiers Received From The WebAPI
|
New features
Universal Import - BETA
These new import options are currently in BETA testing and will be available to all customers soon!
Our Universal Interface Import allows users with an EMR/EHR that has not built an interface with us to import encounter, claim, and patient data from any external system. Customers can now upload CSV, Excel, TSV, and pipe-delimited files using our Interface Import section. This new feature uses AI-powered field mapping to automatically interpret the structure of CSV/Excel files from other systems and map them into CMD. This feature allows customers who do not use our WebAPI to automatically import claims, and patients from any EMR/EHR via a report or export from their software. 
Customers can also manually import claims into our system in the HL7 format or claims from an 837 ANSI file format into CollaborateMD.
For more information visit our Universal Import Help Article.
Enhancements
New Option to Ignore Modifiers Received From The WebAPI
When configuring interfaces, we can currently set up the interface to ignore the price that comes over in the message and use our own pricing instead. This is necessary because CMD, as the billing system, houses the fee schedules and contracts. We also have many defaults & automations around modifiers (specifically situational modifiers), but those rules are not used if modifiers are received from your EMR. Some users do not want this since if the modifiers entered in the EMR are wrong, automations will not work.
In this release, we added new options to the Interface Settings screen (for WebAPI Interfaces) that allows you to ignore modifiers sent via the interface. The new setting "Set modifiers based on the modifiers received from the Interface?" will default to Yes to allow setting the modifiers based on the modifiers received from the interface (just like it does today). Even if this is set to Yes, default and situational modifiers will be used if they are not received from the Interface. When set to No it will ignore the modifiers sent from the interface.

For more information visit our Configure Interface Settings Help Article.
New Option To Get Current Claim Status Through The WebAPI
We previously introduced an API endpoint request that allows users to set the claim status. To allow API vendors to continue building on this capability, we added the ability to retrieve the current claim status. This will return an XML response that includes the Claim Status ID, Claim Location ID, and Claim Status Display value.
Resolutions
Report Performance Issue When Combining Results
We resolved an issue in our Report Viewer where reports, run for multiple customers with the "combine results" option selected, took longer to process compared to running the same report with separate results.
Mark as Fixed Issue in Claim Tracker
Corrected an issue within claim tracker where, when checking the Mark As Fixed checkbox on Intelligent Claim Rejection messages should also mark all of the hidden issues as fixed but instead was flagging issues as "Not Fixed."
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| New Features | |
|---|---|
| New Interface Automations |
New features
New Interface Automations
Our CollaborateMD interface provides a powerful bridge to automatically create patients, appointments, and claims in the CMD application via interface messages (ADT, SIU, DFT). Previously, after a patient appointment or claim was received & created via the interface, users still had to perform manual work such as checking eligibility, reviewing/scrubbing claims, or address verification. Powerful add-on features like Eligibility, Claim Scrubbing, and Address Verification had to be used either through a separate integration with our WebAPI (for Eligibility only) or manually in the application. In this release, these actions can now be automated to occur as soon as the claim, patient, or appointment is received. For more information visit our Manage Interface Automations Help Article.
We added the following new automations that can be enabled and configured within the services section by Auth Reps:
Eligibility Interface Automation
We created 2 new eligibility settings to allow eligibility to be automatically checked when a patient, appointment, or claim is created via the interface:
Automatically check eligibility when an appointment or claim is created over an Interface?
Select Yes if you want an automatic eligibility check when creating an appointment or claim, from an SIU or DFT message received via the interface.
Automatically check eligibility when a patient is created or updated over an Interface?
Select Yes if you want an automatic eligibility check when creating a patient from an ADT message received via the interface.

Claim Scrubbing Interface Automation
We created a new claim scrubbing setting to automatically review claims created via the interface:
Automatically review and scrub new claims as they are entered through an Interface?
Select Yes if you want to automatically scrub new claims created from a DFT message received via the interface.

For more information visit our Manage Claim Scrubbing Help Article.
Address Verification Interface Automation
We created a new Address Verification setting to automatically scrub addresses when creating/editing a patient record via the interface:
Automatically scrub addresses when the above changes are made via Interface?
Select Yes if you want to automatically scrub addresses (based on your pre-selected options) when creating or editing a patient record from an ADT/DFT message received via the interface.

For more information visit our Manage Address Verification Help Article.
Coming Soon - Patient Estimates Interface Automation
The ability to automatically generate patient estimates upon appointment or claim creation via the interface will be added soon!
Resolutions
Claim Control for Large Batches
We resolved an issue within Claim Control that could prevent users from changing the status of more than one thousand claims at once. This action would cause a "Maximum call stack size exceeded" console error when updating the claim status. With this new update, when a user updates claim statuses, it is performed in batches of 1,000 and pre-selects all the remaining claims that exceed 1000 after in initial claim status update. If more than 1,000 claims are selected for saving, a modal will appear stating: "Only 1,000 claims can be saved at once. After the save is complete, the remaining X claims will be selected in the table and can then be saved." Following the save, the selections in the table will be updated accordingly.
Intelligent Claim Rejections Enabled by Default
The Intelligent Claim Rejection feature was enabled for most customers, but an issue prevented its automatic enablement for new submitters. This issue marked the submitter in CMD with the feature turned on without changing the submitter request sent to ePS. In this release, we corrected this issue to ensure that submitter registrations sent to ePS turns this feature flag on.
Intelligent Claim Rejections Enabled by Default
In this release, we corrected some appointment reminder issues where some appointments were not sent and others had expired confirmation tokens. This issue was causing the confirm & cancel links in the appointment reminder to stop working after an additional reminder was sent to the patient.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
Enhancements
New "To Date" Optional Column
We have always displayed the "From" Date (Date of Service) as a column in our Claim Control, Claim Tracking, and Follow-Up Management tables. This represents the first date of service on the claim. Customers who treat patients for extended periods (especially those using Institutional claims) could not view the complete range of service dates in these tables. In this release, we added the "To" Date (representing the last date of service on the claim) as an optional, hidden-by-default column. 
New ERA Warning when Patient Name Doesn't Match
A new ERA Warning has been implemented for instances where the patient's first or last name on the ERA (EraClaim.plast and EraClaim.pfirst) does not match the name recorded in our application. The warning message, "Warning: The patient name as sent by the payer does not match your records," will alert users to this discrepancy.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
| Enhancements | |
|---|---|
| New Referring Provider Note Report Field New Optional Columns in Claim Control & Follow Up Management ERA Claim-level Payments Now Evenly Applied |
Enhancements
New Referring Provider Note Report Field
In this release, we added a new report field for the Referring Provider’s Note text field. This new report field (available under Referring Data) is useful for recording various information. For example, users can note the name of the facility a referring provider is from, allowing them to report on the number of lab samples received from each facility. 
New Optional Columns in Claim Control & Follow Up Management
Some customers use the Account Type and Reference # fields in CMD to store information that does not fit elsewhere in the application. While integrating fields for workflows across different specialties would be ideal, many customer issues can be resolved by allowing them to view this information in various places. In this release, we added these two columns as optional (not visible by default) in both Follow Up Management and Claim Control. 
ERA Claim-level Payments are Now Evenly Applied
Some payers (particularly for institutional claims) send only a claim-level payment rather than line-item payments. Previously, our system applied these payments by distributing as much of the paid amount on each charge as possible, and then as much of the adjusted amount on each charge as possible, resulting in uneven claim application, and requiring users to manually correct the ERAs for institutional claims. With this release, these payments will now be applied evenly.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.
Highlights
New features
Alternate Eligibility Payer ID
Some HMO payers (specifically Independent Physician Associations, or IPAs, in California) have a specific network payer ID that provides claim services, while the regular payer ID is used for Eligibility. Users have previously requested that we update our system to add a separate connection for Eligibility when the main clearinghouse connection doesn’t support Eligibility. In this release, a new checkbox has been added to the patient insurance policy section, allowing users to verify eligibility through an alternative payer. When selected, an additional field appears, enabling users to search for and designate a separate payer. This option is available only when the primary payer does not support eligibility verification. 
For more info on how to set up a different payer ID for eligibility, visit our Add Insured or Payer Policy Help Article.
Universal Import Updates
This release introduces more enhancements to the Universal Import feature to improve data matching accuracy, and reduce manual preparation across various import scenarios. These updates include:
- Anesthesia Support: Previously, customers were required to manually enter start and stop times for each anesthesia claim during the import process. This will now happen automatically while processing Universal Import files. The system now identifies start and stop times, calculates the duration of anesthesia, and automatically applies the appropriate units and pricing based on those minutes.
- Fix Import Data Option: When importing a file, users may receive a warning indicating insufficient information to create patients or claims. The system provides details specifying the requirements needed in the file to resolve these errors. This required the file to be updated and re-uploaded, even if the only change involved a field shared by all patients or claims, such as provider, date of service, or diagnosis. This release introduces a "Fix" button, allowing you to enter missing information directly during the import process. You no longer need to modify and re-import files; you can now update data for all patients or claims directly within the system at the time of import. Please note that this method is only suitable when the missing information is the same across all records, such as a shared diagnosis, procedure code, or date of service. If the missing information varies, you must update the import file accordingly before uploading. This approach applies only when the data is identical for all items imported from the claim.

For more information on using the Fix option, visit our Importing CSV, Excel, TSV, or Pipe-Delimited Files Help Article.
Enhancements
Claim Status Service Information Now Displayed
Previously, electronic claim status responses displayed claim-level payment information but omitted certain charge-level details provided by the payer. Consequently, data such as service line payment amounts were not captured, requiring users to contact the payer directly for this information. In this release, the system will automatically pull in the paid amount for each service line, provided the payer supplies this information. Access to this data will save customers time by eliminating the need to contact the payer for status updates.
New Alerts Column in Claim Control
A new "Alerts" optional column has been added to the Claim Control table, allowing users to view alerts while reviewing claims prior to submission. This column is hidden by default and mirrors the functionality in Follow-Up Management, displaying a clickable yellow bell icon when alerts are present. Clicking the icon displays the claim alert pop-up. 
New Alerts Side Panel in Follow Up Management
This release introduces alert visibility when viewing individual claims within Follow Up Management. Previously, alerts were only accessible via the main table’s yellow bell icon. Users can now view or add alerts directly within the side panel, enabling immediate issue identification during claim processing. 
Visit our View/Add Alerts From Follow Up Help Article for more information.
Charge Panel Limit Increased
Previously, our charge panels were limited to five-character codes, restricting the system to 999 panels. In this release, we have increased the code limit to 10 characters to support a larger volume of panels, allowing customers to create an unlimited number of charge panels per account. 
New Report Field: # of Public Follow Up Notes
Previously, it was possible to retrieve the number of claim notes but not follow-up notes. This release introduces a new report field, "# Number of Public Follow-Up Notes," allowing users to see the number of public claim follow up notes in reports. This release also renames the existing "# Number of Notes" field to "# Number of Claim Notes." 
Resolutions
Denials and Unpaid Reasons Reports Slowness When Using Remittance Received date
Resolved an issue causing slowness in "Denials and Unpaid Reasons" reports when using the Remittance Received date filter. This fix significantly improves the performance of the remittance received report filter for customers.
As part of this release, we are continuing our ongoing work to assess, monitor, and address any security vulnerabilities.