There may be errors, warnings or informational messages present on your ERAs. These can be present for a number of reasons, from CMD not being able to find the charge, to a remittance code warning. CollaborateMD is designed to help you resolve these issues by providing suggestions.
Please review the common ERA Errors Help Article for a list of common ERA Errors and Warnings.
Within the ERA section you will see 5 different informational icons
-
Errors
 : Errors will prevent you from fully posting your ERA payments. ERA errors range from CMD being unable to locate the patient associated with the payment to not being able to locate the charge.
: Errors will prevent you from fully posting your ERA payments. ERA errors range from CMD being unable to locate the patient associated with the payment to not being able to locate the charge. -
Warnings
 : Warnings should be addressed before posting the payment, but will not prevent the system from posting the payment. Warnings range from letting you know the charge is already reporting as paid to the allowed amounts not matching the contracted amount.
: Warnings should be addressed before posting the payment, but will not prevent the system from posting the payment. Warnings range from letting you know the charge is already reporting as paid to the allowed amounts not matching the contracted amount. -
Information
 : Information messages should also be addressed before posting the payment, but will not prevent the system from posting the payment. Information messages are used to inform you on remittance codes on the ERA. They can range from a message letting you know the payer did not pay on a charge to letting you know the service was not covered by the payer.
: Information messages should also be addressed before posting the payment, but will not prevent the system from posting the payment. Information messages are used to inform you on remittance codes on the ERA. They can range from a message letting you know the payer did not pay on a charge to letting you know the service was not covered by the payer. -
Alerts
 : Any Patient, Code, or Payer alert will appear here if they have been configured to appear in the Payment section.
: Any Patient, Code, or Payer alert will appear here if they have been configured to appear in the Payment section. -
Fully Applied Payments
 : This Icon will let you know if the payment associated with this claim has been fully applied.
: This Icon will let you know if the payment associated with this claim has been fully applied.
Address errors, warnings and informational messages within an ERA.
-
Select Payment > ERA.
-
Enter your Search Criteria.
-
Locate the ERA in the results.
-
Click the Start/Continue Review button.
-
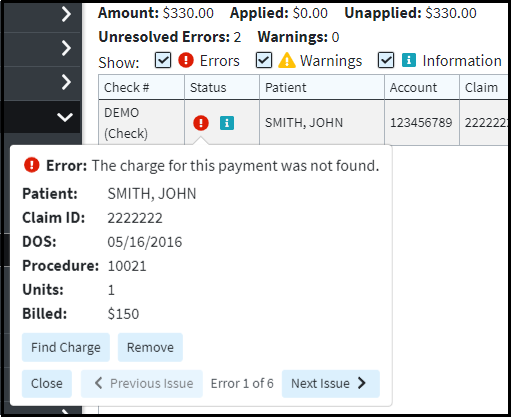
Click on an icon to view the errors, warnings, or information messages.
-
Depending on the error, warming or information messages you'll see the following options.
-
Next Issue: View the next error, warning or informational message associated with this claim.
-
Previous Issue: View the previous error, warning or informational message associated with this claim.
-
Close: Close the pop-up window.
-
Remove: Remove the selected claim, payment or adjustment.
-
Find Charge: Find the charge the payment is associated with.
-
Find TCN: Find the TCN for the claim the payment is associated with.
-
Apply: Apply any secondary or tertiary insurance payments, or apply a refund or reversal.

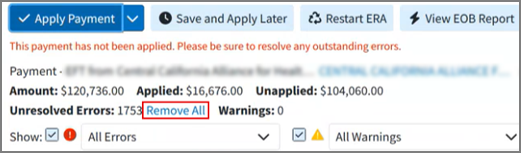
Optional: Remove All: When 2 or more unresolved errors of the type "the claim or patient for this payment was not found" are present, the system will display a "Remove All" button. Clicking this button will remove all such errors simultaneously instead of having to remove them one by one.
-
-
Click the Apply Payment button after resolving and reviewing all errors, warnings and information messages.


