Who can add new providers?
Users with the Account Setup & Providers permissions can add a new Provider with an existing Tax ID.
Users with the Bill Payment, Account Setup & Providers permissions can add a new Provider with a new Tax ID.
Follow the steps below to add a New Provider.
-
Select Customer Setup > Providers.
-
Click the New Provider button.
-
Enter the provider Last Name, First Name, MI & Credentials.
-
Add the provider’s NPI number. Or click the
 icon to search the NPPES NPI Registry for all NPI records of Healthcare Providers.
icon to search the NPPES NPI Registry for all NPI records of Healthcare Providers.-
Once the NPI Registry window opens, select the NPI type.
-
Enter your search criteria and click Search.
 If you're searching with a partial name or are unsure of the spelling, it must be followed by an asterisk * (i.e. When searching for the “James Jones”” type in “Jame*” in the first name field and “Jon*” in the last name field so it pulls up all records that include “Jame” and “Jon” in the first/last name). Failure to add the wildcard (*) will result in the registry only searching for an exact match and may not pull up the record you are searching for.
If you're searching with a partial name or are unsure of the spelling, it must be followed by an asterisk * (i.e. When searching for the “James Jones”” type in “Jame*” in the first name field and “Jon*” in the last name field so it pulls up all records that include “Jame” and “Jon” in the first/last name). Failure to add the wildcard (*) will result in the registry only searching for an exact match and may not pull up the record you are searching for. -
A window will open displaying the NPI numbers that match your search results.
-
Select the NPI of the Provider you would like to add.
-
-
The Sequence # is auto-populated by CollaborateMD.
-
Enter the Taxonomy Specialty that defines the Provider's area of specialization. Or click on the
 icon to select one from the list.
icon to select one from the list. - A Reference # can be created to further identify the provider.
-
Enter a Code you would like to associate with the provider.
-
Use the
 icon to select the Default Practice for this provider.
icon to select the Default Practice for this provider.Important: Once the provider has been saved, the practice listed in this field cannot be changed.
-
For Bill claims under, use the
 icon to select the Billing Provider that should be used for the claim.
icon to select the Billing Provider that should be used for the claim. Leave as SELF if this provider is the Billing Provider.
Leave as SELF if this provider is the Billing Provider. -
Use the
 icon to select the provider to Check eligibility under.
icon to select the provider to Check eligibility under. Leave as SELF if this provider will submit eligibility requests to the payer themselves.
Leave as SELF if this provider will submit eligibility requests to the payer themselves. -
Select which Tax ID number (SS/EIN) this provider will use, and enter it into the field.
 Whenever a new provider with a new Tax ID is added, a prompt appears requesting the details of the authorized signer for the payer agreements associated with this submitter. An authorized signer is an individual designated by the customer/owner to sign and handle payer agreements for a submitter/Tax ID. This authorized signers name, title, and phone number must be entered in order to complete the new provider process.
Whenever a new provider with a new Tax ID is added, a prompt appears requesting the details of the authorized signer for the payer agreements associated with this submitter. An authorized signer is an individual designated by the customer/owner to sign and handle payer agreements for a submitter/Tax ID. This authorized signers name, title, and phone number must be entered in order to complete the new provider process.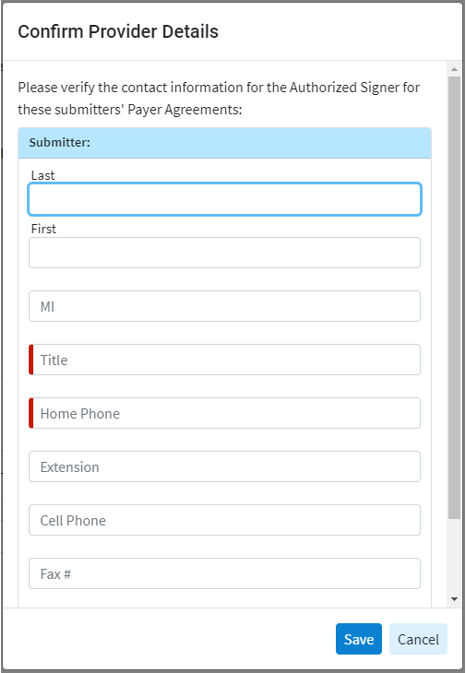
-
Select whether this provider will Bill as an Individual or a Group.
-
Professional Mode/Institutional Mode: Authorized Reps and Admins with the Account Setup permission can move Provider(s) into Production Mode once a Submitter Number is assigned to the Provider(s).
-
Production Mode: Claims will be submitted to the payer for processing.
-
Test Mode: Claims will not be submitted to the payer for processing, and only sent to the Clearinghouse.
-
Hold Mode: Claims will not be submitted to the payer or Clearinghouse. Claims will stay in CollaborateMD.
-
-
Enter the provider’s Contact Information (e.g., phone, fax, cell phone, email).
-
Add any applicable ID Numbers by referencing the Provider Field Descriptions below.
-
Enter any applicable Claim Defaults:
-
Optional: Use the
 icon to select a Default Revenue Code to associate with this provider.
icon to select a Default Revenue Code to associate with this provider. -
Optional: Use the
 icon to select a Default Facility to associate with this provider.
icon to select a Default Facility to associate with this provider. -
Click Save.
Important: If adding a new provider with a new Tax ID, a payment window will be shown to collect the one-time payment. The provider will not be registered with the clearinghouse if the payment fails. Claims cannot be submitted electronically, eligibility cannot be checked, and agreements cannot be started until the provider has been registered.
Once you have corrected the payment information, please open the provider Provider Name (#sequence number) and click the
 button to register the provider.
button to register the provider.
Credentials: The provider’s medical credentials. (MD, OD, RN etc.)
NPI: The provider’s National Provider Identification number.
Taxonomy Specialty: The provider’s Taxonomy code that identifies the provider type and area of specialization.
Sequence#: This number is auto-populated by CollaborateMD. This is an internal number and not appear on the claim.
Reference#: In the event, you have to enter a provider into the system twice, use this field to help distinguish between the two providers. (e.g., Tax ID, EIN, Provider A, Provider B). This field is informational and does not appear on the claim.
Code: You can use this field to enter a code of up to 3 letters or numbers. This code will then be displayed on certain reports within the Report screen of the application to identify which provider performed the service. This code will not appear on any claim.
Practice for this provider: Click on the magnifying glass to search for the practice you want to associate the provider too. This will be the provider's default practice. Important Note: Once the provider has been saved, the practice listed in this field cannot be changed.
Bill claims under: This field defaults to Self. Click on the magnifying glass to choose the provider that should populate in the billing provider field for all future claims.
Check eligibility under: This field defaults to Self. Click on the magnifying glass to choose the provider all eligibility checks will be submitted under. We recommend configuring one provider for all eligibility checks to be completed under to prevent having to configure multiple providers.
Bill as: Select whether this provider will bill under their individual provider (Provider screen) information or group (Practice screen) information.
Use which ID number: Select whether to bill using the provider’s SSN or EIN number.
Submitter Number: The Clearinghouse assigns each new Tax ID number a Submitter Number. This Submitter Number tells the clearinghouse which customer is sending them electronic products such as claims, statements, ERA's, etc. It also allows them to send Clearinghouse reports back into your account. A Submitter Number will automatically be generated under the Internal Use field.
Blue Cross #: Blue Cross assigned number to identify providers.
Tricare/Champus #: Tricare assigned number to identify providers.
Specialty License #: The Referring provider’s Specialty License number.
State License #: The Referring provider’s State License number.
Anesthesia License #: The Referring provider’s Anesthesia License number.
UPIN #: Medicare assigned number to identify providers. This number populates on Box 17a (of the CMS 1500 form)
Default Revenue Code: For UB-04 claims only. Revenue codes are descriptions and dollar amounts charged for hospital services provided to a patient.. Select a default revenue code. The revenue code may change depending on the service provided.
Default Facility: Select a default facility. When a new claim is created, the Provider's default Facility will be used if the Patient doesn't have a default Facility (The Patient's default Facility takes precedence over the Provider's default Facility).
 icon to search the
icon to search the  If you're searching with a partial name or are unsure of the spelling, it must be followed by an asterisk * (i.e. When searching for the “James Jones”” type in “Jame*” in the first name field and “Jon*” in the last name field so it pulls up all records that include “Jame” and “Jon” in the first/last name). Failure to add the wildcard (*) will result in the registry only searching for an exact match and may not pull up the record you are searching for.
If you're searching with a partial name or are unsure of the spelling, it must be followed by an asterisk * (i.e. When searching for the “James Jones”” type in “Jame*” in the first name field and “Jon*” in the last name field so it pulls up all records that include “Jame” and “Jon” in the first/last name). Failure to add the wildcard (*) will result in the registry only searching for an exact match and may not pull up the record you are searching for. icon to select one from the list.
icon to select one from the list. icon to select the Default Practice for this provider.
icon to select the Default Practice for this provider. icon to select the Billing Provider that should be used for the claim.
icon to select the Billing Provider that should be used for the claim. Leave as SELF if this provider is the Billing Provider.
Leave as SELF if this provider is the Billing Provider. icon to select the provider to Check eligibility under.
icon to select the provider to Check eligibility under.
 icon to select a Default Revenue Code to associate with this provider.
icon to select a Default Revenue Code to associate with this provider. button to register the provider.
button to register the provider.